- Grassroots Vitality
- Posts
- Is Leaky Gut Wrecking Your Health?
Is Leaky Gut Wrecking Your Health?
A Science-Backed Guide to Repairing Intestinal Permeability Naturally

🩺 WELLNESS SPOTLIGHT: GETTING TO THE BOTTOM OF LEAKY GUT
Ever wonder why your doctor rolls their eyes at the mention of "leaky gut," while your functional medicine practitioner treats it like the holy grail of diagnoses? Welcome to one of medicine's most fascinating controversies.
When gastroenterologists and functional medicine practitioners debate "leaky gut," they're wrestling with a fascinating paradox in modern medicine. The condition – more formally known as increased intestinal permeability – sits at the intersection of emerging research and clinical uncertainty. But what exactly are we measuring, and why do the standards vary so dramatically across the globe?
The intestinal barrier consists of three key components: a surface mucus layer, the epithelial cell layer, and immune defenses. There are three different pathways in the intestine that control how substances pass between epithelial cells.
Leak Pathway: Allows larger molecules to pass through tight junctions, regulated under normal conditions.
Pore Pathway: Facilitates the transport of ions and small molecules through tight junctions and is highly selective.
Unrestricted Pathway: Linked to disease states, such as cell death, allowing bacteria and other harmful substances to pass through the intestinal barrier unchecked.
Picture your intestinal barrier as an extraordinarily sophisticated security system. Testing for intestinal permeability employs various methods, each with its limitations. Zonulin Testing, which measures zonulin levels in blood or stool, has shown inconsistent results; high serum zonulin is more closely linked to metabolic markers than specific gut issues, leaving its role in diagnosing leaky gut uncertain.
Emerging markers like lipopolysaccharide-binding protein, a toxin produced by certain microbes, are under investigation but are not yet reliable for clinical use.
Elevated fecal calprotectin levels indicate the migration of neutrophils to the intestinal mucosa or even into the gut lumen in cases of gut barrier disturbances.
The Lactulose/Mannitol Test is the most widely utilized method for assessing intestinal permeability, primarily measured through urine collection.
This latter test employs two non-metabolized sugars: lactulose, a larger molecule, and mannitol, a smaller one. The fundamental premise is that lactulose is expected to pass through damaged areas of the intestinal barrier, while mannitol is thought to traverse the intestinal wall through healthy epithelial pathways.
But here's where it gets intriguing:
In Brazilian research published in Scielo, healthy individuals showed lactulose recovery of 0.07%, while celiac patients averaged 0.15%. Crohn's disease patients demonstrated levels of 0.42%. Yet the clinical interpretation of these numbers reveals a striking geographic disparity:
Australian clinicians consider 0.30% their threshold for concern.
U.S. laboratories set their bar significantly higher at 0.90%.
European standards fall somewhere in between.
This variation isn't just academic. At 0.60%, a patient might be considered perfectly healthy in Minneapolis but requiring intervention in Melbourne.
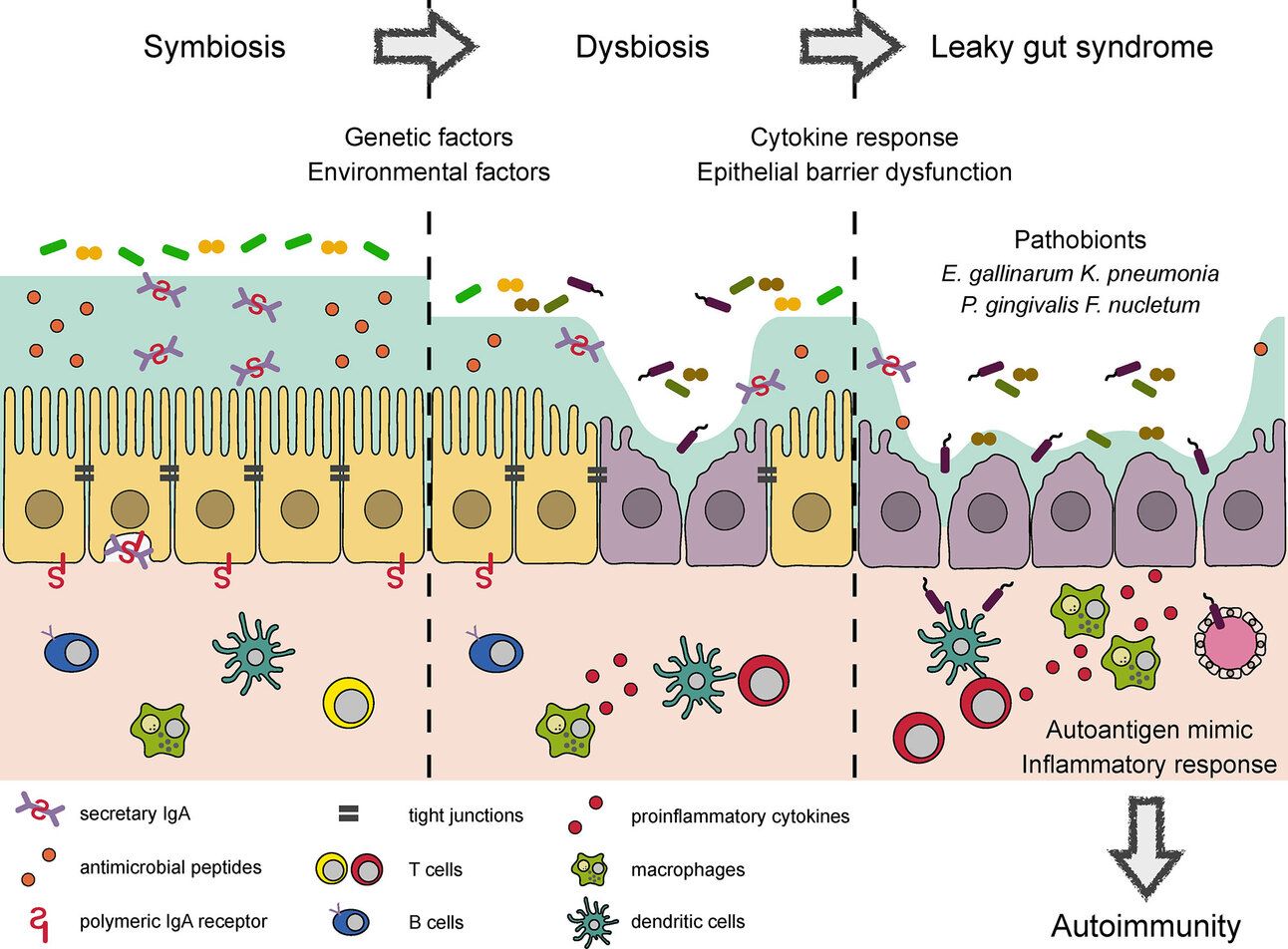
Beyond the Gut: The Bigger Picture
Research shows that abnormal intestinal permeability is present in irritable bowel syndrome (IBS), although the level of permeability is lower than in inflammatory bowel disease (IBD) or celiac disease. Studies suggest that increased permeability may precede flare-ups of Crohn's disease, indicating its role in gut inflammation. Various non-gastrointestinal diseases, including asthma, autism, and multiple sclerosis, have also been associated with leaky gut.
Understanding and Taking Action
When it comes to gut barrier function, timing and triggers matter more than you might think. Your intestinal permeability isn't fixed – it can change rapidly based on your daily choices and exposures. Many common substances can temporarily increase gut permeability, including over-the-counter pain medications (NSAIDs like ibuprofen and aspirin), alcohol, high amounts of saturated fats, and even intense exercise. The good news is that this type of increased permeability often resolves once you remove the triggering factors.
Certain supplements have been proven to support gut integrity and function:
Zinc Carnosine (37.5-75mg daily): Aids in maintaining tight junctions.
L-Glutamine (5-15g daily): Provides fuel for intestinal cell repair.
Probiotics (10-20 billion CFU): Particularly Lactobacillus rhamnosus GG, which has shown effectiveness in improving gut barrier function.
Curcumin (500-2000mg daily): Known for its anti-inflammatory properties.
Colostrum (10-60g daily): Supports mucosal integrity.
Upregulating SCFA Production Shows Particular Promise
Short-chain fatty acids (SCFAs), the byproducts of dietary fiber fermentation, are emerging as metabolic game-changers that play a role in metabolic health indicators like weight, glucose, insulin, and triglycerides. SCFAs are essential metabolites of probiotics, serve as a source of energy for the colonic mucosa, strengthen the intestinal protective barrier, and regenerate the colonic epithelium.
Resistant starch, inulin, xylooligosaccharides (a type of plant fiber), and arabinogalactan (a natural sugar found in plants) are types of dietary fibers and prebiotics that promote the growth of beneficial gut bacteria, particularly those that produce butyrate, a short-chain fatty acid (SCFA) with significant health benefits.
Supporting Gut Barrier Health
Your gut microbiome plays a vital role in maintaining a strong and healthy gut barrier. A balanced microbial community helps protect against inflammation and supports overall gut integrity.
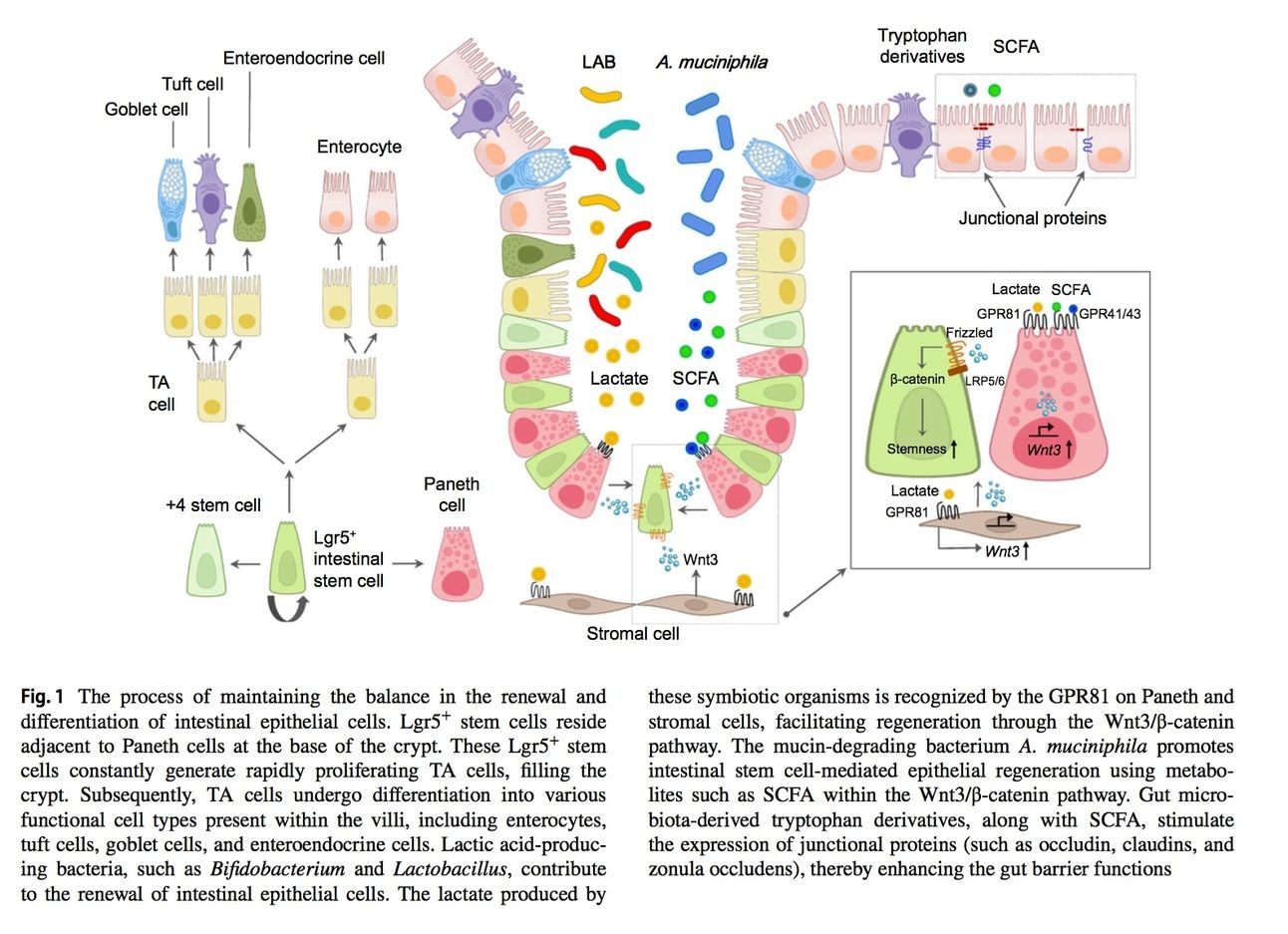
Good Bacteria for Gut Health: Beneficial microbes like Akkermansia muciniphila and butyrate-producing bacteria encourage mucus production and help regulate tight junctions (the "seals" between gut cells).
Harmful Bacteria to Watch For: High levels of Proteobacteria can disrupt this balance, potentially leading to inflammation and a weakened barrier. Bilophilia wadsworthia is a bacteria that is increasingly linked to leaky gut due to its ability to produce hydrogen sulfide, a gas that can damage the intestinal lining.
How to Strengthen Your Gut Barrier: Focusing on boosting butyrate producers such as Faecalibacterium, Blautia, and Roseburia may help maintain gut health.
Closing the Gap on Leaky Gut
Ultimately, the debate over intestinal permeability underscores the complexity of gut health and the evolving nature of medical science. While “leaky gut” may remain a contentious term, there’s no denying that gut barrier integrity plays a crucial role in overall wellness. Whether you approach it from a clinical or functional medicine perspective, the key takeaway is that your intestinal permeability is not static—it responds to diet, lifestyle, and environmental factors. By reducing gut-disrupting triggers and fostering beneficial gut bacteria through food-based choices, you can take meaningful steps toward optimizing your digestive health.
Please note: Some of the links in this newsletter are affiliate links. If you make a purchase through these links, we may earn a small commission at no additional cost to you. Your support helps Grassroots Vitality continue to provide valuable content. Thank you!
🦉DAILY WISDOM: FINDING BALANCE
“In order to heal, it is essential to gather the strength to think negatively. Negative thinking is not a doleful, pessimistic view that masquerades as ‘realism.’ Rather, it is a willingness to consider what is not working. What is not in balance? What have I ignored? What is my body saying no to? Without these questions, the stresses responsible for our lack of balance will remain hidden.”
― Gabor Maté, When the Body Says No

🥦 HEALTHY HACKS: PROTECTING GUT HEALTH DURING & AFTER ANTIBIOTICS
While antibiotics are essential for fighting infections, they can disrupt your gut’s microbial balance—sometimes for years afterwards, depending on the antibiotic. Research suggests that combining probiotics and prebiotic-rich foods can help maintain microbial diversity during treatment. Here’s a quick guide:
1. Probiotics During Antibiotic Use
Probiotics help replenish beneficial bacteria and mitigate the side effects of antibiotics.
Saccharomyces boulardii (Florastor)
Reduces AAD and systemic Candida infections.
Proven to cut AAD risk by over 50% in both children and adults.
Lactobacillus rhamnosus GG (LGG)
Effective in reducing AAD risk, especially in children.
Supports adults undergoing H. pylori eradication therapy.
2. Prebiotics for Post-Antibiotic Recovery
Prebiotics are fibers that nourish beneficial bacteria, helping to restore gut diversity. Dr. Jason Hawrelak, a prominent microbiome specialist, suggests that consuming prebiotics for 6 weeks post-treatment can help reestablish lost gut diversity.
Inulin and FOS (4–10 g): Found in garlic, onions, chicory root, and Jerusalem artichokes.
Galactooligosaccharides (3.5–7 g): Present in legumes, chickpeas, and lentils.
Acacia Gum (5–10 g): Supports growth of bifidobacteria and lactobacilli.
Partially Hydrolyzed Guar Gum (PHGG) (5–10 g): Promotes butyrate production for gut healing.
HMO prebiotics fuel beneficial gut bacteria like Bifidobacteria and Akkermansia, promoting better digestion, immunity, and overall wellness. Learn more more about the benefits of Layer Origin.

💊 SUPPLEMENT SAVVY: HARNESSING ELDERBERRY FOR DIGESTIVE HEALTH
A recent clinical trial examined the effects of one week of elderberry juice consumption on gut health and metabolism in 18 healthy adults. The study, titled Elderberry Juice Modulates Gut Microbiota Composition and Improves Glucose Tolerance in Healthy Adults: A Randomized Controlled Trial, uncovered several significant benefits:
Key Findings:
Enhanced Gut Microbiota: Significant increases in beneficial bacteria, particularly Bifidobacterium and Lactobacillus species.
Better Glucose Control: 24% lower glucose response after meals, with a 9.9% reduction in insulin sensitivity.
Improved Fat Metabolism: 27% increase in fat oxidation, suggesting potential benefits for weight management.
Practical Application:
Consume 300 mL of elderberry juice daily – the amount used in the study to achieve these results.
Study Limitations and Future Directions:
Results appear unique to elderberry juice and not replicated with mixed-berry alternatives, suggesting specific benefits from elderberry's compounds.
One-week duration limits understanding of long-term effects; longer studies needed to confirm sustained benefits.
🥛 BETTER HABITS: BIFIDO YOGURT FOR HISTAMINE SENSITIVITY
If you're sensitive to Lactobacillus or experience brain fog from fermented dairy, try this homemade Bifidobacteria yogurt. This specialized yogurt avoids the use of Lactobacillus found in all store-bought yogurts and ensures it primarily ferments Bifidobacteria, making it ideal for people with MCAS, histamine intolerance, or SIBO.
Ingredients:
Milk (UHT or sterilized)
Prebiotics: FOS (1 tsp to 1 tbsp per liter), 2-FL (human milk oligosaccharide), Arabinogalactan, Acacia, GOS, PHGG, XOS
Probiotic culture: SeekingHealth Probiota Bifido
Optional: Lactase enzymes for lactose-free yogurt
Method:
Heat milk to 185°F (85°C) for 20 minutes. Cool to 100°F (38°C).
Stir in prebiotic of choice.
Add SeekingHealth Probiota Bifido and mix.
Optional: Add lactase enzyme for lactose-free.
Incubate at 100°F for 24-36 hours.
Enjoy creamy, Bifidobacteria-only yogurt. Discard or drink the whey.
This yogurt is a simple, gut-friendly option for those with specific sensitivities, offering unique probiotic benefits without the unwanted side effects of other strains.
Make pure, probiotic-rich yogurt at home with Luvele Yogurt Makers. Their new Pure and Pure Plus models feature Water-Bath Technology for even temperature control, ensuring optimal probiotic growth. With a 36-hour timer and adjustable temperature (25-50°C), you can perfect your yogurt every time. Learn more.

📰 HEALTH HEADLINES
From groundbreaking studies to ancient wellness practices, here are the latest insights into natural health and healing.
⚡ Gut Microbiome Regulates Brain Signals Through the Vagus Nerve
🍹 I’ve been drinking kombucha for years and it’s transformed my gut health – here’s how
🧠 Gut bacteria can alter brain proteins: New glycosylation method uncovers link
🦠 Scientists Just Discovered Why Antibiotics Struggle To Eliminate Certain Infections
🔗 COMMUNITY PULSE POLL: SHARE YOUR GUT HEALTH SECRETS!
Have a wellness journey to share? I’d love to feature your story—reach out and inspire others with your experience! Feel free to leave a comment below 😃
If this issue resonates with you, share it with your community to get the word out!
See you next week! 👋
Reply